Periodontal vs. Gingivitis: Understanding the Differences

Regarding dental health, two common terms often arise gingivitis and periodontal disease. Both conditions relate to the health of your gums, but they are not the same. According to the Centers for Disease Control and Prevention (CDC), nearly 47% of adults over 30 suffer from some form of periodontal disease. Knowing the differences between these two conditions is essential for proper treatment and prevention. This article will explain the differences, causes, symptoms, and treatments of gingivitis vs periodontal disease. What Is Gingivitis? Gingivitis is the mildest form of gum disease. It’s an early stage where the gums become inflamed due to plaque buildup on the teeth. Gingivitis is reversible with proper care, making it essential to catch and treat it early. The primary cause of gingivitis is poor oral hygiene. When you don’t brush or floss regularly, plaque, a sticky film of bacteria, forms on your teeth. Over time, this plaque irritates your gums, leading to inflammation and bleeding during brushing or flossing. The good news is that gingivitis can be controlled with regular brushing, flossing, and professional cleanings. What Is Periodontal Disease? If gingivitis is left untreated, it can progress to a more severe condition known as periodontal disease. The CDC reports that periodontal disease affects nearly 70% of adults aged 65 and older. This condition is much more serious because it involves the gums and the bones supporting your teeth. Once periodontal disease advances, it can lead to tooth loss if not treated promptly. Periodontal disease occurs when plaque spreads below the gum line. The bacteria in plaque produce toxins that irritate the gums and cause inflammation. This inflammation causes the gums to pull away from the teeth, forming pockets. These pockets become infected, and as the disease progresses, the bones, gums, and connective tissue that support the teeth are destroyed. Without treatment, the teeth may eventually become loose and fall out. Symptoms: How to Identify Gingivitis vs Periodontal Disease It’s important to recognize the symptoms of gingivitis and periodontal disease to seek timely treatment. Here’s how you can differentiate between these two: Gingivitis Symptoms: Red, swollen gums that bleed easily during brushing or flossing. The gums may feel tender, but there’s usually no pain at this stage. You might also notice bad breath (halitosis). Periodontal Disease Symptoms: Symptoms are more severe and may include receding gums, deep pockets between teeth and gums, loose or shifting teeth, pus between the teeth and gums, and persistent bad breath. As the disease progresses, you may experience pain while chewing, and your teeth may become loose or fall out. Causes of Periodontal vs Gingivitis Disease Understanding the causes of gingivitis and periodontal disease can help you prevent these conditions. According to the World Health Organization (WHO), gum diseases are the 11th most prevalent disease globally. The causes can vary, but some common factors include: Poor Oral Hygiene: The most common cause of gingivitis is poor oral hygiene. Not brushing and flossing regularly allows plaque to build up, leading to inflammation of the gums. Smoking: Tobacco use is a significant risk factor for periodontal disease. Smokers are seven times more likely to develop gum disease than non-smokers. Hormonal Changes: Women may experience gum inflammation during pregnancy, menstruation, or menopause due to hormonal fluctuations. Medical Conditions: Certain diseases, such as diabetes, can increase the risk of developing gum disease. People with diabetes are more likely to develop infections, including periodontal disease. Medications: Some medications can reduce saliva flow, leading to a dry mouth and increasing gum disease risk. Learn more about Gingivitis: Does Hydrogen Peroxide Cure Gingivitis? Exploring Its Role in Oral Health Treatment Options: What Can Be Done for Periodontal vs Gingivitis? When treating gingivitis and periodontal disease, the earlier you start, the better. For gingivitis, the treatment is straightforward. Good oral hygiene is often enough to reverse the condition. Regular brushing, flossing, and professional cleanings can remove plaque and prevent gingivitis from worsening. Your dentist may also recommend an antibacterial mouthwash to reduce plaque and bacteria. For periodontal disease, the treatment depends on the severity of the condition. In the early stages, scaling and root planning can be effective. This deep cleaning removes plaque and tartar below the gum line and smooths the tooth roots to help the gums reattach. Surgical treatments like flap surgery, bone grafts, or tissue regeneration may be necessary if the disease has advanced. What Happens If Left Untreated Periodontal vs Gingivitis? Ignoring gingivitis or periodontal disease can have serious long-term consequences. The CDC states that gum disease is the leading cause of tooth loss in adults. Without proper treatment, gingivitis can progress to periodontal disease, leading to irreversible damage to your gums and the supporting structures of your teeth. Untreated Gingivitis: If left untreated, gingivitis can lead to periodontitis, which can cause the gums to recede and form pockets. These pockets can infect and destroy the tissue and bone supporting your teeth. This process can result in tooth loss and may even affect your overall health, as periodontal disease has been linked to conditions like heart disease, diabetes, and respiratory issues. Untreated Periodontal Disease: The consequences are even more severe. As the disease progresses, the pockets deepen, and more gum tissue and bone are destroyed. Teeth may become loose and eventually fall out or need to be removed. Advanced periodontal disease can also lead to systemic issues, as the bacteria from the infection can enter the bloodstream and affect other parts of the body. Conclusion: Taking Control of Your Gum Health Gum health is vital to your overall well-being. According to the ADA, untreated gum disease can lead to serious health problems, including heart disease and stroke. Understanding the difference between gingivitis and periodontal disease is the first step in taking control of your gum health. You can prevent gum disease and maintain a healthy smile by practising good oral hygiene, quitting smoking, and visiting your dentist regularly. Remember, early detection is key to preventing the progression
Understanding the Dangers of a Tooth Infection
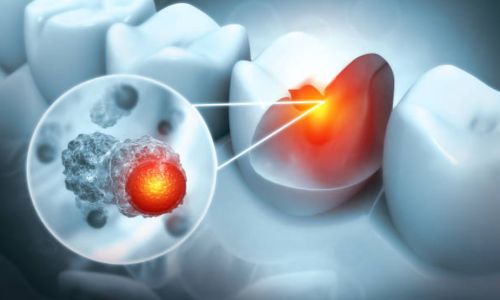
Tooth infections, if left untreated, can pose serious health risks, potentially leading to life-threatening complications. This article will explore tooth infection kills, the associated risks, and the importance of timely intervention. What is a Tooth Infection? A tooth infection, also known as a dental abscess, occurs when bacteria invade the tooth’s pulp, forming pus. This can result from untreated cavities, cracked teeth, or gum disease. The infection can cause significant pain, swelling, and other symptoms, indicating the need for immediate dental care. Symptoms of a Tooth Infection Recognizing the symptoms of a tooth infection is crucial for seeking timely treatment. Common symptoms include: Severe Toothache A persistent, throbbing toothache is one of the most common and noticeable symptoms of a tooth infection. This pain can be quite severe and continuous, making it difficult to ignore. The pain is often described as sharp or shooting and may intensify when you lie down. The toothache may also radiate to the jawbone, neck, or ear on the same side as the infected tooth. This discomfort is typically a result of the infection spreading to the nerves in the tooth’s root, causing inflammation and intense pain. Swelling Swelling is another prominent symptom of a tooth infection. The gums around the affected tooth may become swollen, red, and tender. This swelling can extend to the face or jaw, leading to visible puffiness and discomfort. In some cases, the swelling can be so significant that it causes difficulty in opening the mouth, eating, or speaking. This symptom indicates the infection has spread beyond the tooth and affects the surrounding tissues. Fever A fever may develop as your body’s immune system fights the infection. An elevated body temperature indicates that your body responds to the bacterial invasion. Along with fever, you might experience general malaise, fatigue, and feeling unwell. A fever suggests that the infection is more severe and that medical attention is needed promptly. Bad Breath: Tooth Infection Kills Bad breath, also known as halitosis, is a common symptom of a tooth infection. The pus and decaying tissues within the infected tooth can lead to a foul smell or taste in your mouth. This unpleasant odour persists despite regular brushing and mouthwash use. It is often a clear indication of an underlying infection that needs to be addressed. Sensitivity Increased sensitivity to hot or cold temperatures can indicate a tooth infection. You might feel sharp pain when consuming hot drinks, cold foods, or even when breathing in cold air. This sensitivity occurs because the infection irritates the nerve endings within the tooth, making it more reactive to temperature changes. Swollen Lymph Nodes The lymph nodes under your jaw or neck may become swollen and tender when a tooth infection occurs. These nodes are part of your body’s immune system and become enlarged as they work to fight off the infection. Swollen lymph nodes can be painful to the touch and a sign that the disease spreads beyond the tooth. Complications of Untreated Tooth Infection Kills If a tooth infection is left untreated, it can spread to other parts of the body, leading to severe and potentially fatal complications: Abscess Spread If a tooth infection is left untreated, the disease can spread from the tooth to the surrounding tissues, forming a larger abscess. This can lead to increased pain, swelling, and more severe infection. An abscess is a pocket of pus that can cause significant discomfort and may need to be drained by a dentist. Bone Infection (Osteomyelitis) Bacteria from a tooth infection can spread to the bones supporting the teeth, causing a condition known as osteomyelitis. This infection of the bone can cause severe pain, swelling, and fever. Osteomyelitis requires prompt medical treatment, often including antibiotics and sometimes surgery, to remove the infected bone tissue. Cellulitis A tooth infection can spread to the skin and soft tissues, leading to cellulitis. This serious bacterial infection causes redness, swelling, and pain in the affected area. Cellulitis can spread rapidly and become life-threatening if it enters the bloodstream. Immediate medical treatment is essential to prevent severe complications. Sepsis If a tooth infection spreads to the bloodstream, it can lead to severe and potentially fatal sepsis. Sepsis is the body’s extreme response to an infection and can cause widespread inflammation, leading to organ failure and septic shock. Symptoms of sepsis include high fever, rapid heart rate, difficulty breathing, and confusion. Sepsis is a medical emergency that requires immediate treatment in a hospital. Sepsis is a leading cause of death in the United States, with a mortality rate of over 215,000 deaths per year. Source. Ludwig’s Angina Ludwig’s angina is a type of severe cellulitis that occurs on the floor of the mouth. It causes swelling, difficulty breathing, and difficulty swallowing and can rapidly become life-threatening. This condition requires emergency medical treatment, including antibiotics and sometimes surgery, to secure the airway and treat the infection. How Long Until a Tooth Infection Kills? The timeline for a tooth infection to become life-threatening can vary widely depending on several factors, including the individual’s overall health, the severity of the disease, and how quickly it spreads. In some cases, a tooth infection can lead to severe complications very rapidly, while in other cases, it might take weeks or even months to progress to a life-threatening stage. Immediate Danger: Tooth Infection Kills Sometimes, a tooth infection can quickly escalate, leading to severe symptoms such as difficulty breathing or swallowing. These symptoms are medical emergencies and require immediate attention. Rapid progression can be especially dangerous for individuals with weakened immune systems or other underlying health conditions. Gradual Progression The infection may cause persistent symptoms for many people that gradually worsen over time. The disease can spread to surrounding tissues and other body parts without treatment, leading to serious health issues. Regular monitoring and early intervention are key to preventing the disease from reaching a critical stage. Importance of Timely Treatment To prevent complications, seeking prompt dental care at the first sign of a
How to Have Beautiful Teeth

Beautiful teeth not only enhance your smile but also boost your confidence. Achieving and maintaining a radiant smile involves a combination of good oral hygiene, regular dental visits, and a healthy lifestyle. Understanding how to have beautiful teeth can help you enjoy a stunning smile for years. “A gap-free smile is considered more attractive by 90% of people surveyed.” Sources Importance of Beautiful Teeth Beautiful teeth play a significant role in your overall appearance and self-esteem. A bright, white smile can make a positive impression and enhance your confidence in social and professional settings. Healthy teeth also contribute to better oral health, reducing the risk of cavities, gum disease, and other dental issues. Prioritizing your dental care can lead to a more attractive and healthier smile. Practicing Good Oral Hygiene Good oral hygiene is the foundation of beautiful teeth. Regular brushing, flossing, and rinsing help remove plaque and prevent cavities. Proper oral hygiene also keeps your gums healthy, reducing the risk of gum disease. Incorporating these habits into your daily routine is essential for maintaining a bright and healthy smile. Brushing Brushing your teeth twice daily is crucial for removing food particles and plaque. Use a fluoride toothpaste and a soft-bristled toothbrush. Brush for at least two minutes, making sure to clean all surfaces of your teeth. Pay special attention to the gum line, as plaque can accumulate and cause gum disease. Flossing Flossing helps remove plaque and food particles between your teeth, which your toothbrush can’t reach. Floss at least once daily, using a gentle sawing motion to avoid injuring your gums. Proper flossing can prevent cavities and gum disease, creating a healthier and more beautiful smile. Rinsing Rinsing with an antiseptic mouthwash can help kill bacteria and freshen your breath. Mouthwash can also reduce plaque and prevent gum disease. Rinse your mouth with mouthwash after brushing and flossing to enhance your oral hygiene routine and keep your teeth and gums healthy. Regular Dental Visits Regular dental visits are essential for maintaining beautiful teeth. Your dentist can detect and address dental issues early, preventing them from becoming more severe. Professional cleanings remove plaque and tartar buildup, keeping your teeth clean and healthy. Regular check-ups also allow one to discuss concerns and receive personalized advice on maintaining your smile. Professional Cleanings Professional cleanings remove plaque and tartar that brushing and flossing can’t reach. Your dentist or hygienist will use specialized tools to clean your teeth thoroughly, including below the gum line. Regular cleanings prevent cavities, gum disease, and other dental issues, contributing to a healthier and more attractive smile. Dental Check-Ups Regular dental check-ups allow your dentist to monitor your oral health and detect any issues early. During a check-up, your dentist will examine your mouth, gums and mouth for signs of cavities, gum disease, and other problems. Early detection and treatment can prevent more severe issues and help maintain your beautiful smile. Healthy Diet and Lifestyle A healthy diet and lifestyle play a crucial role in maintaining beautiful teeth. Certain foods and habits can affect oral health, so making mindful choices is essential. Avoiding sugary foods and drinks, staying hydrated, and quitting smoking can significantly impact the health and appearance of your dentures. Avoid Sugary Foods and Drinks Sugary foods and drinks can contribute to tooth decay and cavities. Bacteria in your mouth feed on sugar, producing acids that erode your tooth enamel. Limit your consumption of sugary snacks, candies, and sodas. Opt for healthier alternatives like fruits, vegetables, and water. Stay Hydrated Staying hydrated is essential for your overall health and oral health. Drinking plenty of water helps rinse away food particles and bacteria, reducing the risk of cavities and gum disease. Water also stimulates saliva production, which helps neutralize acids and protect. Quit Smoking Smoking can significantly negatively impact your oral health and the appearance of your teeth. Tobacco use can cause yellowing, staining, and bad breath. It also increases the risk of gum disease and oral cancer. Quitting smoking can improve health and contribute to a more beautiful smile. Teeth Whitening Teeth whitening is a popular cosmetic procedure that can enhance the appearance of your smile. There are various methods available, including professional treatments and at-home options. Understanding the benefits and risks of teeth whitening can help you make an informed decision. Professional Teeth Whitening Your dentist performs professional teeth whitening and offers the most effective results. The procedure typically involves applying a bleaching agent and using a special light to enhance the whitening process. Professional whitening can lighten your teeth in just one visit, providing a brighter and more radiant smile. At-Home Teeth Whitening At-home teeth whitening kits are available over the counter and can be a convenient option for enhancing your smile. These kits usually include whitening strips, gels, or trays you apply to your teeth. While at-home treatments may not be as effective as professional whitening, they can still provide noticeable results. It’s essential to follow the instructions carefully to avoid potential side effects. Correcting Dental Issues Correcting dental issues is essential for achieving and maintaining beautiful teeth. Misaligned, chipped, or missing can affect the appearance of your smile and your oral health. Various treatments, including orthodontics, veneers, and dental implants, are available to address these issues. Orthodontics Orthodontic treatments, such as braces and clear aligners, can correct misaligned teeth and improve your bite. Straightening your teeth enhances your smile and makes it easier to clean your teeth and maintain good oral hygiene. Orthodontic treatments can significantly improve the appearance and health. Veneers Veneers are thin shells of porcelain or composite resin bonded to the front of your incisors. They can correct cosmetic issues, including discolouration, chips, and gaps. Veneers provide a natural-looking solution for enhancing the appearance of your smile. Dental Implants Dental implants are a permanent solution for replacing missing tooth. They consist of a titanium post that is surgically placed into your jawbone and a crown that is attached to the post. Dental implants look and function like natural
Inflamed Gums After Flossing: Causes, Prevention, and Treatment

Maintaining oral hygiene is essential for healthy teeth and gums. Flossing is a crucial part of this routine, yet many people experience inflamed gums after flossing. This article explores the reasons behind inflamed gums, how to prevent them, and effective treatment methods. Understanding Inflamed Gums After Flossing Flossing is designed to remove plaque and food particles from between teeth, where a toothbrush cannot reach. However, if you experience inflammation after flossing, it can be concerning. Inflamed gums are characterized by redness, swelling, and sometimes bleeding. This reaction can be due to various factors. Common Causes of Inflamed Gums After Flossing Several factors can cause inflamed gums after flossing. Understanding these can help prevent and manage the condition effectively. Incorrect Flossing Technique One of the primary reasons for inflamed gums is incorrect flossing technique. Using too much force or snapping the floss between teeth can injure the gum tissue, leading to inflammation. Gums are sensitive and need gentle care, even when flossing. Gingivitis Gingivitis is the inflammation of the gums due to plaque buildup along the gumline. If you have not been flossing regularly, the sudden introduction of flossing can irritate as it removes plaque and bacteria, leading to temporary inflammation. Tartar Buildup If plaque is not removed regularly, it hardens into tartar, irritating and inflaming the gums. Flossing can disturb this tartar, causing the gums to become inflamed. Allergic Reactions In some cases, an allergic reaction to the floss material can cause gum inflammation. This is less common but still a possible cause. Underlying Dental Conditions Certain dental conditions, such as periodontitis or abscesses, can cause inflammation. Flossing can exacerbate these issues, leading to inflamed gums. Prevention Strategies for Inflamed Gums After Flossing Preventing inflamed gums after flossing involves adopting proper techniques and maintaining overall oral hygiene. Here are some effective strategies: Use the Correct Flossing Technique Ensure you are flossing correctly. Use a gentle sawing motion to guide the floss between your teeth. Curve the floss into a C-shape around each tooth and gently slide it under the gumline. Avoid snapping the floss, as this can damage your gums. Floss Regularly Consistency is key in maintaining healthy gums—Floss at least once daily to remove plaque and food particles before they harden into tartar. Regular flossing helps prevent gum inflammation. Inflamed Gums After Flossing: Choose the Right Floss Select a floss that suits your needs. If you have sensitive gums, consider using a softer floss or a waxed version to reduce irritation. There are also flosses designed for people with braces or dental work. Rinse Your Mouth After flossing, rinse your mouth with water or an antibacterial mouthwash. This helps remove any dislodged particles and reduces the risk of inflammation. Brush Properly Brushing your teeth twice daily with a soft-bristled toothbrush helps maintain oral hygiene. Use fluoride toothpaste to strengthen your teeth and gums. Ensure you brush gently along the gumline to remove plaque without causing damage. Stay Hydrated Drinking plenty of water helps keep your mouth clean and your gums healthy. Water flushes out food particles and bacteria that can cause inflammation. Treatment for Inflamed Gums After Flossing If you experience inflamed gums despite preventive measures, there are several treatments you can consider. These treatments help alleviate symptoms and promote healing. Saltwater Rinse A simple saltwater rinse can reduce inflammation and promote healing. Mix half a teaspoon of salt in warm water and rinse your mouth for 30 seconds. Repeat this twice a day until the inflammation subsides. Cold Compress Applying a cold compress to the outside of your cheek can reduce swelling and numb the pain. Use a cold pack or a bag of frozen peas wrapped in a cloth. Apply it for 15-20 minutes several times a day. Over-the-Counter Anti-Inflammatories Non-prescription anti-inflammatory medications, such as ibuprofen, can help reduce pain and inflammation. Follow the dosage instructions and consult your dentist if you have any concerns. Topical Treatments Over-the-counter gels and creams designed for oral use can help soothe inflamed gums. Look for products containing benzocaine or hydrogen peroxide. Apply as directed on the package. Professional Dental Cleaning If tartar buildup is causing your gum inflammation, professional dental cleaning is necessary. Your dentist or dental hygienist will remove the tartar and plaque, reducing inflammation and preventing future buildup. Consult Your Dentist If your symptoms persist despite home treatments, consult your dentist. Persistent inflammation can be a sign of an underlying dental condition that requires professional attention. Your dentist can diagnose the issue and recommend appropriate treatment. Importance of Regular Dental Checkups Regular dental checkups are essential for maintaining oral health and preventing gum inflammation. During these visits, your dentist can identify and treat any potential issues before they become serious problems. Early Detection of Gum Disease Regular checkups allow your dentist to detect early signs of gum disease, such as gingivitis before it progresses to more severe conditions like periodontitis. Early treatment can prevent complications and keep your gums healthy. Professional Cleanings Professional cleanings remove plaque and tartar that regular brushing and flossing cannot. These cleanings help prevent gum inflammation and maintain overall oral health. Personalized Oral Care Advice Your dentist can provide personalized advice on oral care, including proper flossing techniques and the best products for your needs. This guidance can help prevent inflamed gums and other dental issues. When to Seek Immediate Dental Care if Inflamed Gums After Flossing While mild gum inflammation after flossing can be managed at home, certain symptoms require immediate dental attention. These include: Severe pain Persistent bleeding Swelling that does not subside Pus discharge from the gums Fever These symptoms can indicate a serious infection or other dental issues that need prompt professional treatment. The Role of Diet in Gum Health A balanced diet plays a crucial role in maintaining healthy gums. Certain nutrients are essential for gum health; incorporating them into your diet can help prevent inflammation. Vitamin C Vitamin C is essential for healthy gums. It helps in collagen production, which is crucial for gum tissue.
How to Prepare a Tooth for a Crown
Getting a dental crown is a common procedure in modern dentistry. Crowns restore a tooth’s shape, strength, and function after damage. Whether the damage is due to decay, a large filling, or a fracture, a crown can help protect and strengthen the tooth. This article will walk you through the detailed steps of how to prepare a tooth for a crown, ensuring you understand the entire process. Understanding Dental Crowns Dental crowns are caps placed over a tooth to restore shape, size, and appearance. They can be made from various materials, including metal, porcelain, resin, or ceramic. Crowns are used for multiple reasons, such as to protect a weak tooth, restore a broken tooth, cover a dental implant, or improve the appearance of a discolored or misshapen tooth. Types of Dental Crowns There are different types of dental crowns, each with its benefits. Metal crowns, made from gold, platinum, or base-metal alloys, are known for their durability and strength. Porcelain-fused-to-metal crowns provide a more natural tooth color and are suitable for front and back teeth. All ceramic or all-porcelain crowns offer the best natural color match and are ideal for people with metal allergies. Resin crowns are less expensive but wear down over time and are more prone to fractures. Initial Consultation for Prepare a Tooth for a Crown The first step in preparing a tooth for a crown is an initial consultation with your dentist. During this visit, your dentist will examine the tooth and determine if a crown is the best option for treatment. They will take X-rays to assess the roots of the tooth and the surrounding bone. If the tooth has extensive decay or there is a risk of infection, a root canal treatment may be necessary before the crown is placed. Treatment Plan: Prepare a Tooth for a Crown Your dentist will develop a treatment plan based on the examination and X-rays. This plan will outline the steps to prepare your tooth for a crown. It will also include details about the type of crown used and the procedure’s timeline. Your dentist will discuss the treatment plan with you and address any questions or concerns you may have. Prepare a Tooth for a Crown Once the treatment plan is in place, the next step is to prepare the tooth for the crown. This involves several key steps to ensure the tooth is properly shaped and ready for the crown to be placed. Anesthesia to Prepare a Tooth for a Crown The first step in the preparation process is administering local anesthesia to numb the tooth and surrounding area. This ensures you do not feel any pain during the procedure. Your dentist will use a needle to inject the anesthesia into the gums near the tooth that will receive the crown. Removing Decay and Old Fillings After the anesthesia takes effect, your dentist will remove any decay from the tooth. If the tooth has an old filling, it will also be removed. This step is crucial to ensure the tooth is free of decay or infection before placing the crown. Reshaping the Tooth When Prepare a Tooth for a Crown Next, the dentist will reshape the tooth to make room for the crown. They will trim the tooth on the top and sides using a dental drill. The amount of teeth removed depends on the type of crown being used. For example, metal crowns require less tooth removal than porcelain or ceramic crowns. The goal is to create a tooth shape that allows the crown to fit snugly and securely. Building Up the Tooth Sometimes, the tooth must be built up before the crown can be placed. This is often necessary if a large portion of the tooth is missing due to decay or damage. Your dentist will use a filling material to build up the tooth’s core, providing a solid foundation for the crown. Taking Impressions to Prepare a Tooth for a Crown After the tooth is properly shaped, impressions are taken. These impressions create a custom crown that fits perfectly over the prepared tooth. Digital Impressions Many modern dental offices use digital impression technology to create a 3D image of the tooth. This process involves using a small wand to scan the tooth and surrounding area. The digital images are then sent to a dental lab, where the crown is designed and manufactured. Digital impressions are more accurate and comfortable than traditional impressions. Traditional Impressions In some cases, traditional impressions may be used. This involves placing a putty-like material in a tray and pressing it against the tooth. The material sets and creates a mold of the tooth. The mold is then sent to a dental lab, where the crown is made. While traditional impressions are effective, they can be uncomfortable for some patients. The global dental crowns and bridges market size was valued at USD 2.85 billion in 2018 and is projected to reach USD 4.56 billion by 2026. Source. Temporary Crown Placement While waiting for the permanent crown, your dentist will place a temporary crown over the prepared tooth. This temporary crown protects the tooth and maintains its function until the permanent crown is ready. Creating the Temporary Crown The temporary crown is usually made from acrylic or composite resin. Your dentist will shape the material to fit over the prepared tooth. It is then cemented in place with temporary dental cement. The temporary crown is not as strong as the permanent crown, so avoiding chewing hard or sticky foods that could dislodge it is important. Caring for the Temporary Crown While you have a temporary crown, it is important to take care of it to avoid any issues. Avoid chewing on the side of the mouth with the temporary crown, and practice good oral hygiene by brushing and flossing gently around the crown. If the temporary crown becomes loose or falls off, contact your dentist immediately to have it re-cemented. Permanent Crown Placement Once the permanent crown is ready, you will return
Does Amoxicillin Help Wounds Heal Faster?
Introduction of Amoxicillin as an antibiotic The quest for faster wound healing is a topic of significant interest in healthcare. Wounds can be painful and inconvenient from injury, surgery, or other causes. Many individuals seek ways to accelerate the healing process, and one question that arises is whether antibiotics like amoxicillin can aid in this endeavor. In this article, we will explore the role of amoxicillin in wound healing. Does amoxicillin help wounds heal faster? What is its mechanism of action, what are its potential benefits, and what are some important considerations? All these questions are answered here: Understanding Amoxicillin Helps Wounds Heal Faster: Amoxicillin belongs to a class of antibiotics known as penicillins. It is widely prescribed for treating various bacterial infections, ranging from respiratory tract infections to skin and soft tissue infections. Amoxicillin works by inhibiting the growth of bacteria, ultimately leading to their death. It achieves this by interfering with the synthesis of bacterial cell walls, weakening the bacteria’s structural integrity and making them more susceptible to the body’s immune defenses. The Role of Antibiotics in Wound Healing: When it comes to wound healing, antibiotics play a crucial role in preventing or treating infections. Infections can impede the healing process by prolonging inflammation, causing tissue damage, and delaying the formation of new tissue. By targeting and eliminating harmful bacteria present in or around the wound, antibiotics help create a favorable environment for healing to occur. However, it’s important to note that not all scars require antibiotics, and their use should be guided by a healthcare professional based on factors such as the type, severity, and risk of infection associated with the wound. Does Amoxicillin Specifically Promote Faster Wound Healing? While amoxicillin can effectively combat bacterial infections, its direct role in accelerating wound healing needs clarification, such as topical agents or growth factors specifically designed to enhance wound healing processes; amoxicillin primarily targets bacteria rather than directly stimulates tissue repair. That being said, by resolving or preventing bacterial infections, amoxicillin indirectly supports the body’s natural healing mechanisms, allowing it to operate more efficiently. Potential Benefits of Using Amoxicillin for Wound Healing: Although amoxicillin may not directly speed up wound healing, its use can offer several potential benefits in the context of wound management: Infection Prevention: One of the primary benefits of using amoxicillin in wound care is its ability to prevent or treat infections. By eliminating harmful bacteria that could otherwise compromise the healing process, amoxicillin helps reduce the risk of complications and promotes optimal wound healing. Reduced Inflammation: Infections are often accompanied by inflammation, which can exacerbate pain, swelling, and tissue damage. Amoxicillin can help mitigate inflammation by resolving bacterial infections, allowing the body’s natural healing mechanisms to function more effectively. Enhanced Comfort: Wounds that become infected are typically more painful and uncomfortable. By addressing bacterial infections promptly, amoxicillin can alleviate discomfort associated with wound-related infections, improving the overall patient experience during the healing process. Facilitated Tissue Repair: While not a direct effect of amoxicillin, the resolution of bacterial infections can indirectly support tissue repair by creating a more conducive environment for the proliferation and migration of cells involved in wound healing, such as fibroblasts and keratinocytes. Adults, teenagers, and children weighing 40 kilograms (kg) or more—250 to 500 milligrams (mg) every 8 hours, or 500 to 875 mg every 12 hours. Important Considerations for Does Amoxicillin help wounds heal faster Despite the potential benefits of using amoxicillin for wound healing, several important considerations should be kept in mind: Antibiotic Resistance: The widespread use of antibiotics has contributed to the emergence of antibiotic-resistant bacteria, posing a significant global health threat. To mitigate the risk of antibiotic resistance, it is essential to use antibiotics judiciously and only when necessary. Healthcare professionals should carefully evaluate the need for antibiotics in wound management and consider alternative strategies where appropriate. Allergic Reactions: Amoxicillin belongs to the penicillin class of antibiotics, and individuals with a known allergy to penicillin or other beta-lactam antibiotics should avoid its use. Allergic reactions to amoxicillin can range from mild skin rashes to life-threatening anaphylaxis, necessitating prompt medical attention. Side Effects of Using Amoxicillin on Wounds to Heal Faster: Like all medications, amoxicillin can cause side effects, including gastrointestinal disturbances such as nausea, vomiting, diarrhea, and abdominal pain. While these side effects are generally mild and transient, they can impact patient compliance and overall treatment outcomes. Consultation with Healthcare Professionals: The decision to use amoxicillin for wound healing should be made in consultation with a healthcare professional, such as a physician or wound care specialist. These professionals can assess the wound’s specific characteristics, evaluate the risk of infection, and determine the most appropriate course of treatment based on individual patient needs. Conclusion: Does Amoxicillin Help Wounds Heal Faster While amoxicillin is an effective antibiotic for treating bacterial infections, its role in promoting faster wound healing is indirect. Amoxicillin helps create an optimal environment for wound healing by targeting and eliminating bacterial pathogens. However, its use should be guided by healthcare professionals and based on the specific clinical context of the wound. As with any medication, the potential benefits of using amoxicillin for wound healing must be weighed against the risks, including antibiotic resistance and possible side effects. Comprehensive wound management requires a multidisciplinary approach considering various factors to optimize patient outcomes. Amoxicillin and Wound Healing: FAQs for Dental Patients Q: Does amoxicillin help wounds heal faster after a dental procedure? Amoxicillin is an antibiotic whose primary benefit is preventing infection in wounds, not necessarily speeding up healing itself. After a dental procedure, especially one that involves a surgical incision (like wisdom tooth removal), your dentist might prescribe amoxicillin to reduce the risk of bacteria entering the wound and causing complications. Q: When would a dentist prescribe amoxicillin after a dental procedure? There are several factors a dentist considers when deciding if amoxicillin is necessary: Type of procedure: Surgeries, deep cleanings (scaling and root planing), or procedures on patients with a high risk of
Does Hydrogen Peroxide Cure Gingivitis? Exploring Its Role in Oral Health

Gingivitis, a common gum disease characterized by inflammation of the gums, affects millions of people worldwide. If left untreated, it can cause discomfort and bleeding and even lead to more severe oral health issues. In the quest for effective home remedies, many have turned to hydrogen peroxide as a potential solution. But does hydrogen peroxide really cure gingivitis? Let’s explore this question and understand the role of hydrogen peroxide in oral health. What is Hydrogen Peroxide? Hydrogen peroxide (H2O2) is a chemical compound of hydrogen and oxygen. It is a colorless liquid with strong oxidizing properties, commonly used as a disinfectant and bleaching agent. You might have encountered it in your household as a solution for cleaning wounds or whitening teeth. The Role of Hydrogen Peroxide in Oral Health Hydrogen peroxide has been used for decades in dentistry for its antibacterial properties. It can help kill harmful bacteria contributing to gingivitis and other oral health issues when applied to the gums. Additionally, it can help reduce inflammation and promote gum tissue healing. Using Hydrogen Peroxide for Gingivitis Many wonder whether using hydrogen peroxide as a mouthwash can effectively treat gingivitis. While hydrogen peroxide can help kill bacteria and reduce inflammation, it is essential to use it correctly and in moderation. Here’s a simple and safe way to use hydrogen peroxide for gingivitis: Dilute the hydrogen peroxide: Pure hydrogen peroxide can be too harsh and may cause irritation or damage to the delicate tissues in your mouth. It’s best to dilute it with equal water to reduce its strength. Swish the solution in your mouth: Take a small amount of the diluted hydrogen peroxide solution and swish it around your mouth for about 30 seconds to one minute. Be sure not to swallow the solution. Spit out the solution: After swishing, spit out the solution and rinse your mouth thoroughly with water to remove any remaining hydrogen peroxide. Repeat daily: For best results, use the hydrogen peroxide mouthwash once a day as part of your oral hygiene routine. However, it’s essential not to overdo it, as excessive use may lead to irritation or damage to the gums. The concentration of hydrogen peroxide in store-bought teeth whitening kits can be as high as 10%. While hydrogen peroxide can be a helpful tool in whitening teeth, it’s important to use it correctly to avoid damaging your gums or tooth enamel. Always follow the directions on the package and consult with your dentist before using any teeth whitening product. Source. Other Tips for Maintaining Oral Health While hydrogen peroxide can be a helpful addition to your oral care routine, it’s essential to remember that it is not a substitute for regular brushing, flossing, and professional dental cleanings. Here are some additional tips for maintaining good oral health: Brush your teeth twice a day: Use fluoride and soft-bristled toothpaste to remove plaque and bacteria from your teeth and gums. Floss daily: Flossing helps remove food particles and plaque from between your teeth, where your toothbrush can’t reach. Visit your dentist regularly: Schedule regular dental checkups and cleanings to detect oral health issues early and prevent gingivitis and other gum diseases. Eat a balanced diet: Limit sugary and acidic foods and beverages, as they can contribute to tooth decay and gum disease. Instead, choose a diet rich in fruits, vegetables, and whole grains. Can You Rinse Away Gingivitis with Hydrogen Peroxide? The answer is not so clear-cut. While some studies suggest hydrogen peroxide might reduce gum inflammation, others haven’t found significant benefits. Here’s why: Limited Effect: Hydrogen peroxide’s antibacterial effect might be temporary and may not reach all the bacteria hiding below the gum line. Potential Irritation: Undiluted or improperly diluted hydrogen peroxide can irritate your gums, worsening the problem. Short-Term Solution: Even if it temporarily reduces inflammation, hydrogen peroxide doesn’t address the root cause of gingivitis—plaque buildup. Safer and More Effective Solutions: So, what can you do to tackle gingivitis effectively? Here are some proven strategies: Brushing: Brush your teeth twice daily for two minutes, using a soft-bristled brush and fluoride toothpaste. Pay close attention to the gum line. Flossing: Floss daily to remove plaque and food particles from between your teeth. Regular dental checkups: Schedule regular dental cleanings to remove built-up plaque and tartar (hardened plaque) that brushing and flossing can’t reach. Your dentist can also identify and address any underlying issues contributing to gingivitis. When to Consider Hydrogen Peroxide (with Caution): If your dentist recommends using a hydrogen peroxide rinse as part of your gingivitis treatment plan, here’s what to keep in mind: Strict Dilution: Only use a solution diluted according to your dentist’s instructions, typically 1.5% to 3% hydrogen peroxide mixed with equal parts water. Short-Term Use: Don’t use a hydrogen peroxide rinse for extended periods, as it can disrupt the natural balance of bacteria in your mouth. Sensitivity Watch: If you experience discomfort, stop using the rinse immediately and consult your dentist. Conclusion of does hydrogen peroxide cure gingivitis While hydrogen peroxide can help kill bacteria and reduce inflammation in the gums, it is not a guaranteed cure for gingivitis. It should be part of a comprehensive oral care routine that includes brushing, flossing, and regular dental checkups. If you suspect you have gingivitis or any other oral health issue, it’s essential to consult with your dentist for proper diagnosis and treatment. With appropriate care and attention to oral hygiene, you can maintain healthy gums and a beautiful smile for years. At Worthy Smiles, we understand the importance of maintaining healthy gums for a beautiful smile and overall well-being. Our experienced team is dedicated to providing preventive care, including thorough cleanings and personalized oral hygiene knowledge. If you experience any signs of gingivitis, we will work with you to develop a treatment plan to restore your gum health and keep your smile shining brightly. Schedule an appointment today, and let us guide you towards optimal oral health! Faqs Q: Is hydrogen peroxide a cure for gingivitis? A: No, hydrogen peroxide isn’t a guaranteed
The Science Behind Fluoride: Protecting Your Enamel
Introduction Enamel, the protective outer layer of our teeth, plays a crucial role in maintaining oral health. In dental care, fluoride has emerged as a key player in enamel protection and preventing decay. However, various factors, including poor dental hygiene and dietary choices, can lead to enamel erosion and compromise our dental well-being. In this article, we delve into the science behind fluoride and its role in safeguarding the enamel of your teeth. Understanding Enamel: The Guardian of Your Teeth Before we explore the protective effects of fluoride, it’s essential to understand the significance of enamel. Enamel is the hard outer layer of teeth that shields them from daily wear and tear, bacteria, and acids produced by plaque. Despite its resilience, enamel is not invincible, and exposure to acids and bacteria can lead to its erosion. This is where fluoride becomes a powerful ally in the battle against enamel deterioration. The Enamel Protection Cycle: How Fluoride Works Fluoride and Mineralization One of the primary mechanisms through which fluoride protects enamel is by promoting remineralization. When our teeth are exposed to acids, minerals such as calcium and phosphate are leached from the enamel. Fluoride helps replenish these lost minerals, contributing to the remineralization process. This strengthens the enamel and makes it more resistant to future acid attacks. Dental Plaque Disruption Fluoride also interferes with the activities of harmful bacteria in dental plaque. These bacteria produce acids that can erode enamel over time. By disrupting the plaque’s ability to generate acid, fluoride acts as a preventive barrier, reducing the risk of enamel damage. Investing in oral health prevention programs yields significant returns, with every $1 invested generating up to $5 in cost savings. (Source: World Health Organization) Fluoride in Oral Care Products: Choosing Your Defense Toothpaste: A Daily Dose of Protection When it comes to enamel protection, your choice of toothpaste matters. Many toothpaste brands incorporate fluoride into their formulations specifically for its enamel-strengthening properties. Look for products that carry the American Dental Association (ADA) seal, ensuring they meet the organization’s standards for safety and efficacy. Mouthwash and Fluoride Treatments In addition to toothpaste, fluoride mouthwashes and professional fluoride treatments provided by dental professionals can further enhance enamel protection. These products deliver a concentrated dose of fluoride, offering an extra defence against enamel erosion. Enamel Protection: Fluoride and Community Water Fluoridation Community water fluoridation is a widespread practice that involves adjusting the fluoride levels in public water supplies. This public health initiative has proven to be a cost-effective way to provide systemic enamel protection to entire communities. Studies have consistently shown a reduction in tooth decay in areas with optimally fluoridated water. Chronic gum disease affects nearly half of adults aged 30 and above, significantly impacting overall health and well-being. (Source: American Dental Association) Best Ways to Enamel Protection Ensuring the protection of enamel is vital for maintaining strong and healthy teeth. Here are some of the best ways to safeguard and fortify your enamel: Brushing with Fluoride Toothpaste: Choose a toothpaste that contains fluoride, a mineral renowned for its enamel-strengthening properties. Brush your teeth at least twice daily, especially after meals, to remove plaque and bacteria that can erode enamel. Enamel Protection: Proper Brushing Technique Use a soft-bristled toothbrush to avoid abrasive damage to the enamel. Brush gently in a circular motion, covering all surfaces of your teeth, including the front, back, and chewing surfaces. Flossing Regularly: Floss daily to remove plaque and debris between teeth and along the gumline where your toothbrush may not reach effectively. This helps prevent cavities and protects the enamel in hard-to-reach areas. Balanced Diet: Consume a well-balanced diet rich in vitamins and minerals, especially calcium and phosphorus, essential for enamel health. Limit the intake of acidic and sugary foods and beverages, as they can contribute to enamel erosion. Drink Water and Chew Sugar-Free Gum: Drink plenty of water throughout the day to help neutralize acids in the mouth and promote saliva production. Chewing sugar-free gum after meals can stimulate saliva flow, aiding in the remineralization of enamel. Regular Dental Check-ups: Schedule regular dental check-ups and cleanings to monitor the health of your enamel and address any emerging issues promptly. Professional dental cleanings help remove stubborn plaque and tartar that may contribute to enamel erosion. Fluoride Mouthwash: Enamel Protection Incorporate fluoride mouthwash into your oral care routine, especially if you are at a higher risk of developing cavities. Swishing with fluoride mouthwash can provide additional protection against enamel damage. Avoid Teeth Grinding: If you grind your teeth (bruxism), consider wearing a nightguard to prevent excessive wear and tear on your enamel. Addressing stress and anxiety, common causes of teeth grinding, can also contribute to enamel protection. Quit Smoking and Limit Alcohol Intake: Smoking and excessive alcohol consumption can contribute to enamel staining and erosion. Quitting smoking and moderating alcohol intake can positively impact enamel health. Community Water Fluoridation: If available in your area, consume tap water, as community water fluoridation is a proven method for enhancing enamel protection at a population level. Remember that consistency is key when it comes to enamel protection. Incorporating these practices into your daily routine and maintaining regular dental visits can contribute to your enamel’s long-term health and resilience. Conclusion: Enamel Protection Understanding the science behind enamel protection is crucial to maintaining optimal oral health. Fluoride, with its remarkable ability to promote remineralization and disrupt the activities of enamel-damaging bacteria, stands as a stalwart defender of our teeth. From daily oral care products to community-wide water fluoridation efforts, incorporating fluoride into our routines plays a pivotal role in safeguarding the integrity of our enamel. So, the next time you reach for your toothbrush, remember that you’re not just cleaning your teeth – you’re actively defending the fortress that is your enamel, ensuring a brighter, healthier smile for years to come. Frequently Asked Questions (FAQs) About Enamel Protection and Fluoride: Q1: What is enamel, and why is it important? A1: Enamel is the hard outer layer of our
Braces, Invisalign, or Clear Aligners: Which Is Right for You?
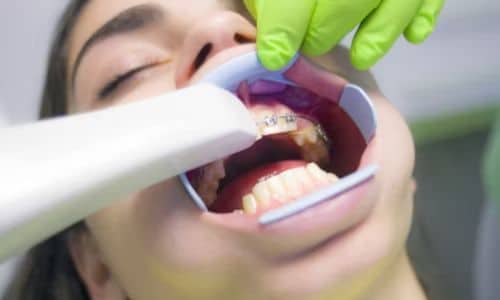
Introduction When achieving a straighter, more confident smile, the options seem endless. Braces, Invisalign, and clear aligners are all effective treatments, but which suits you? In this article, we will explore these orthodontic solutions in detail, providing insights based on expertise and real-life experiences to help you make an informed decision. So, let’s dive into the world of orthodontics and find the perfect solution for your smile transformation. Whether you have crooked teeth, gaps, or bite issues, braces have long been a popular choice for orthodontic treatment. Traditional braces consist of metal brackets and wires that gradually shift your teeth into alignment. Invisalign and clear aligners, on the other hand, offer a more discreet option with removable, custom-made trays to fit your teeth. Let’s explore the pros and cons of each treatment to help you determine which one suits your needs best. Braces: A Time-Tested Classic Braces have been a tried-and-true method for straightening teeth for decades. They consist of metal or ceramic brackets bonded to your teeth, connected by wires that gradually shift your teeth into their desired positions. Braces are known for their effectiveness in correcting complex dental issues such as severe overcrowding or misalignment. However, they can be more noticeable and may require more frequent visits to the orthodontist for adjustments. How Braces Work Braces apply continuous pressure on your teeth, forcing them to move over time. The adjustments made by your orthodontist ensure a precise and effective realignment. The pressure exerted by braces stimulates the bone surrounding your teeth, allowing it to remodel and accommodate the new positions. This gradual movement helps achieve a straighter and healthier smile. Additionally, modern braces come in various options, such as clear or ceramic brackets, making them less noticeable than traditional metal braces. Pros of Braces Highly effective for complex dental issues. Braces are especially beneficial for correcting overcrowding, misalignment, and bite problems. They can also help improve oral health by making cleaning and maintaining proper hygiene easier. Additionally, braces can enhance facial aesthetics and boost self-confidence by giving you a beautiful and aligned smile. Suitable for patients of all ages. Braces are not limited to children and teenagers; adults can also use them. Regardless of age, anyone can benefit from braces to achieve a healthier and more attractive smile. Moreover, advancements in orthodontic technology have made braces more comfortable and less invasive, ensuring a more pleasant experience for patients of all ages. Covered by many insurance plans. This makes braces a more affordable option for patients, as they may be partially or fully covered by insurance. It is essential to check with your insurance provider to understand the extent of coverage for orthodontic treatment. Additionally, some orthodontic practices offer flexible payment plans to make braces more accessible to patients without insurance coverage. Cons of Braces Visible metal or ceramic brackets. These brackets can be noticeable and may affect the appearance of the patient’s smile. However, advancements in orthodontic technology have led to the development of more discreet options, such as clear aligners, which are virtually invisible. Regular adjustments may cause discomfort. However, the discomfort experienced during adjustments is usually temporary and can be managed with over-the-counter pain relievers. Additionally, orthodontists are trained to minimize discomfort during adjustments by using gentle techniques. Dietary restrictions (e.g., avoiding certain foods). Dietary restrictions, such as avoiding sticky or hard foods, may be necessary to prevent damage to the aligners. However, clear aligners offer the advantage of being removable, allowing individuals to enjoy their favorite foods without restrictions during meal times. Invisalign: The Virtually Invisible Option Invisalign, on the other hand, offers a more discreet approach to teeth straightening. These clear plastic aligners are custom-made for your teeth and gradually shift them into place. Invisalign aligners are virtually invisible, making them a popular choice for individuals who want to straighten their teeth without drawing attention to their treatment. Additionally, the custom-made nature of Invisalign aligners ensures a comfortable fit and allows for easy removal when eating or cleaning. How Invisalign Works Invisalign uses a series of clear, removable aligners that you change every two weeks. They are almost invisible and can be easily removed for eating and cleaning. The aligners gradually shift your teeth into the desired position using gentle and controlled force. This allows for a more comfortable and convenient teeth-straightening experience than traditional braces. Pros of Invisalign Virtually invisible, providing aesthetic appeal. Invisalign aligners are also more comfortable to wear than traditional braces, as they are made of smooth plastic and do not have any sharp edges or wires that can irritate. Additionally, since the aligners are removable, you can enjoy your favorite foods without restrictions. Removable for eating and oral hygiene. This means you can easily remove the aligners when you need to eat or brush your teeth, making it easier to maintain good oral hygiene throughout your treatment. Moreover, Invisalign aligners are custom-made for each individual, ensuring a precise and personalized fit for optimal results. No dietary restrictions. Invisalign aligners allow you to maintain your regular diet without any restrictions. This means you can enjoy all your favorite foods and beverages without worrying about damaging or staining your aligners. Smooth and comfortable aligners. Invisalign aligners are made from a soft and comfortable material that won’t irritate your gums or cheeks. This makes them more comfortable to wear throughout the day, allowing you to go about your daily activities without discomfort. According to the manufacturer, teenagers using Invisalign for their orthodontic treatment are twice as likely to have a boost in their self-esteem than those with fixed braces. Cons of Invisalign Not suitable for complex orthodontic issues. Invisalign may not be the best option for individuals with severe bite problems or complex orthodontic issues that require more extensive treatment. In such cases, traditional braces or other orthodontic methods may be recommended to achieve the desired results. Requires discipline to wear aligners consistently. Invisalign requires high discipline to wear the aligners consistently, which must be worn for at least 20-22 hours
When Buying a Manual Toothbrush: What to Look For?
Introduction Choosing the right manual toothbrush might seem simple, but it plays a crucial role in maintaining oral hygiene. With many options available, making an informed decision is essential to ensure your teeth and gums stay healthy. This comprehensive guide will explore what to look for when buying a manual toothbrush, providing expert insights and practical advice. We will explore the different types of bristles, handle designs, and additional features that can enhance your brushing experience. Additionally, we will discuss the importance of replacing your toothbrush regularly and proper brushing techniques to maximize its effectiveness. When Buying a Manual Toothbrush, What to Look For? When buying a manual toothbrush, you must consider several factors to ensure it effectively maintains oral health. Firstly, consider the type of bristles. Dentists recommend soft bristles as they are gentle on your gums and tooth enamel. Secondly, look for a toothbrush with a comfortable handle design for easy maneuverability and control while brushing. Lastly, consider additional features such as a tongue cleaner or gum stimulator, which can benefit your oral hygiene routine. Let’s explore these factors in detail: Bristle Type Matters The type of bristles on your toothbrush can significantly impact your brushing experience. Opt for soft bristles to prevent gum damage and enamel wear. Medium and stiff bristles may be too abrasive for most individuals, potentially causing more harm than good. In addition, consider the size and shape of the strands. Smaller, compact bristles can more effectively reach tight spaces between teeth and along the gumline. On the other hand, more prominent strands may provide a more gentle and comfortable brushing experience. Size and Shape of the Head A toothbrush with a small head allows for better maneuverability, reaching tight spaces in your mouth, such as the back molars. A giant charge, on the other hand, may cover a larger surface area and make brushing quicker and more efficient. It ultimately depends on personal preference and the specific needs of your oral hygiene routine. A compact head is also ideal for individuals with a more petite mouth. Bristle Pattern for Efficient Cleaning Consider toothbrushes with bristle patterns designed for efficient cleaning. Crisscross or angled bristles effectively remove plaque and debris from all tooth surfaces. Handle Grip and Comfort A toothbrush with a comfortable grip ensures a secure hold while brushing. Look for non-slip handles and ergonomic designs that make brushing a breeze, especially for children or those with dexterity issues. Additionally, toothbrushes with rubber grips can provide extra stability and control. This mainly benefits individuals with difficulty gripping objects or limited hand strength. Material and Durability Buying a Manual Toothbrush made from durable materials that can withstand daily use. Quality materials ensure that your toothbrush lasts longer, reducing the need for frequent replacements. Toothbrushes made from nylon bristles are known for their durability and ability to clean teeth effectively. Additionally, toothbrushes with sturdy handles made from plastic or bamboo can contribute to the toothbrush’s overall longevity. Replaceability and Reminder Bristles Some toothbrushes come with reminder bristles that fade over time, indicating when it’s time for a replacement. These bristles help you track when to change your toothbrush, ensuring optimal oral hygiene. Furthermore, toothbrushes with replaceable heads are another option, as they allow you to swap out the worn-out bristles instead of replacing the entire toothbrush. This feature is beneficial for those who often forget to change their toothbrushes every three months, as recommended by dentists. ADA Seal of Approval To ensure the toothbrush meets industry standards, look for the American Dental Association (ADA) Seal of Approval. The ADA Seal of Approval guarantees that the toothbrush has undergone rigorous testing and meets the highest quality and safety standards set by dental professionals. This seal indicates that the toothbrush effectively removes plaque and maintains good oral health. This seal guarantees the toothbrush’s safety and effectiveness. Brand Reputation Opt for well-known and reputable toothbrush brands. These brands often invest in research and development to provide the best oral care products. They also tend to have a broader range of toothbrush options, allowing you to find one that suits your preferences and needs. Additionally, reputable brands often have customer reviews and recommendations to help you decide which toothbrush to purchase. Eco-Friendly Options If you’re environmentally conscious, explore eco-friendly toothbrush options from sustainable materials like bamboo or recycled plastics. These eco-friendly toothbrushes are better for the environment and offer the same effectiveness in cleaning your teeth as traditional toothbrushes. By choosing an eco-friendly option, you can contribute to reducing plastic waste and promote sustainability in your oral care routine. Cost-Effective Choices While it’s tempting to splurge on a high-end toothbrush, plenty of budget-friendly options offer excellent oral care. Evaluate your budget and choose accordingly. Remember that the cost of a toothbrush does not necessarily determine its quality or effectiveness. Many affordable toothbrushes are durable and have bristles designed to clean your teeth effectively. Additionally, opting for a budget-friendly toothbrush can help you save money in the long run, as you can replace it regularly without breaking the bank. Compatibility with Toothpaste Ensure that your chosen toothbrush is compatible with your preferred toothpaste. Some toothbrushes are designed with specific types of toothpaste for optimal results. Using a toothbrush compatible with your select toothpaste can enhance its effectiveness and improve oral hygiene. It is essential to check the packaging or consult your dentist to ensure that the toothbrush and toothpaste work well together, allowing you to achieve the desired results. The 8 Best Toothpastes of 2023 (verywellhealth.com) Travel-Friendly Features Frequent travelers should consider compact and travel-friendly toothbrushes with protective cases or covers. These features help to keep the toothbrush clean and prevent it from getting damaged during travel. Additionally, travel-friendly toothbrushes often have smaller, more lightweight designs, making them easier to pack and carry around. Child-Friendly Designs If you’re buying a toothbrush for a child, look for fun and colorful designs that encourage them to brush regularly. Child-sized handles provide a comfortable grip for small hands. Some toothbrushes for children


